Executive Summary
The United States spends far more on health care than any other advanced economy while delivering weaker performance on affordability, disease prevention, and fiscal sustainability. Although the U.S. leads the world in medical innovation, international evidence shows that its high spending is driven primarily by elevated unit prices rather than excessive utilization or uniquely generous care. Common explanations—such as malpractice liability, fee-for-service medicine, or insufficient government involvement—do not account for the magnitude or persistence of these cost and outcome gaps.
The core structural driver of U.S. health care inflation is the exclusion of employer-sponsored health insurance from taxation, a policy rooted in World War II wage controls and expanded in 1954. This exclusion subsidizes insurance rather than care, suppresses wages, weakens consumer price sensitivity, and entrenches employers as inefficient intermediaries in health care financing. International comparisons—most notably Switzerland’s system of universal, individually purchased insurance—demonstrate that competitive private coverage can achieve lower costs, better outcomes, and stronger fiscal discipline. A sustainable U.S. reform strategy therefore requires a gradual, voluntary transition away from employer-based coverage toward a competitive individual market, combined with targeted reforms to the Affordable Care Act, adoption of proven Swiss-style mechanisms, and modernization of payment rules to enable innovation and prevention.
KEY POLICY RECOMMENDATIONS
Repair the individual market. Expand ACA age-rating flexibility to attract younger enrollees and stabilize risk pools; create a permanent reinsurance program for high-cost patients; fully appropriate cost-sharing reduction subsidies to lower premiums; and improve program integrity and income verification.
Reduce the role of employers as health insurance middlemen. Repeal the ACA employer mandate; expand and codify Individual Coverage Health Reimbursement Arrangements (ICHRAs); move Federal Employee Health Benefits Program enrollees into the individual market; and begin a voluntary transition away from employer-sponsored insurance.
Reduce Medicaid churn and inefficiencies. Migrate able-bodied adults from Medicaid expansion into ACA marketplaces; align subsidies to reduce coverage disruptions and lower long-term costs.
Adopt proven Swiss-style reforms. Enable longer-term insurance contracts to reward prevention; and allow collective price negotiation to counter provider and drug monopolies.
Increase opportunities for innovation within Medicare. Require the highest-income future seniors to obtain coverage outside Medicare, opening space for market-driven innovation; liberalize payment rules to enable care delivery innovation.
Introduction
One of the most widely discussed features of the U.S. economy is that that American health care is significantly costlier than that of other industrialized countries, without generally better health outcomes.
Each year, the Foundation for Research on Equal Opportunity (FREOPP) evaluates the health care systems of the 32 nations with the highest gross domestic product per capita and a population over 5 million, in a survey called the World Index of Healthcare Innovation (WIHI). In the 2024 survey, the U.S. ranked 7th overall: first in Science & Technology but dead last in Fiscal Sustainability. On more detailed measures, the U.S. ranked 22nd on disease prevention and last on affordability of health coverage.
Many theories have been offered as to why American health care is so expensive. Almost all of them are wrong.
Some argue, for example, that the U.S. has a “free-market” health care system, and that this is why American health care is so expensive. But nearly half of U.S. health care spending is government spending; indeed, on a per-capita basis, no country subsidizes health care more than the United States. In 2022, the U.S. subsidized $7,438 of health care per person, compared to the WIHI median of $3,144.
Furthermore, there are a number of countries whose health care systems are more free-market-oriented than America’s, such as Switzerland and Ireland, who enjoy both lower costs and better outcomes relative to the United States. In the WIHI survey, Switzerland and Ireland rank 6th and 1st, respectively, on disease prevention. Others argue that fee-for-service health care is the primary culprit, because, it is said, charging patients on a fee-for-service basis incentivizes doctors and hospitals to prescribe more services in order to capture more revenue. But many other advanced nations use fee-for-service payments and spend far less on health care than the U.S., including Canada, Japan, France, and Germany.
Indeed, several widely cited studies show that the volume of health care utilization in the United States is lower than that of other industrialized countries, but that unit prices of health care in America are far higher. For similar reasons, malpractice litigation and “defensive medicine”—the practice of prescribing additional tests to avoid lawsuits—contribute modestly to higher U.S. health spending.
The single biggest driver of high U.S. health care costs—the original sin of U.S. health care–turns out to be the decision in the mid-20th century to exclude the value of employer-sponsored health insurance from all taxation. The problem is not that Americans experience third-party payment for health care services through insurance. That happens all around the world. The problem is that Americans experience third-party payment of insurance—that is to say, third-party payment of third-party payment of health care: effectively, ninth-party health care.
The original sin of U.S. healthcare: The ESI tax exclusion
In 1942, President Franklin Delano Roosevelt signed into law the Stabilization Act of 1942, which required employers to adhere strictly to a federally controlled schedule of salaries and wages for U.S. workers. Congress and the president were concerned that, with young American men off to war, employers would raise wages to compete for increasingly scarce workers, leading to a wage-price spiral and an inflation crisis.
Employers quickly found a workaround. The wage control system did not account for fringe benefits like health insurance. Employers began offering health insurance as a way of competing for those scarce workers. In 1943, the Internal Revenue Service ruled that these benefits were exempt from taxation. As more and more Americans became subject to the federal income tax, employer-sponsored health insurance became more popular. By 1945, 32 million Americans had employer-sponsored coverage—30 percent of the population—compared to 1.3 million in 1940.
The World War II-era loophole limited the value of the health insurance benefit to 5 percent of a worker’s salary. But in 1954, within an overhaul of the Internal Revenue Code, Congress excluded the value of employer-sponsored health insurance from all taxation, including federal, state, and local income taxes, as well as Medicare and Social Security payroll taxes.
The exclusion from taxation of employer-sponsored insurance (hereafter “the ESI exclusion”) effectively forced workers to become dependent upon their employers for health insurance. Imagine a worker in the 22 percent federal tax bracket, paying a 4 percent state income tax and 7.65 percent in FICA, for a total of 33.65 percent. That worker keeps 66.35 cents after tax for every additional dollar received in wages. But that same dollar, if spent on employer-sponsored health insurance, is worth 100 cents: a 51 percent premium.
Over time, this 51 percent premium for compensation spent on health insurance had several pernicious inflationary effects:
- Cost insensitivity and lack of price transparency. Because workers’ health benefits are taken out of their paycheck pre-tax, they usually have no idea how much they are paying (indirectly) for health insurance. This means that they are unaware that rising health insurance premiums are depressing their wages, and lack the agency to shop for less-costly, higher-value coverage.
- Conflict of interest between employers and workers. Workers have an incentive to shop for the best value when it comes to their health benefits: a high-quality plan at an affordable price. Employers, on the other hand, are concerned about keeping their workers away from competitors by offering generous benefits, and incentivized to become passive about cost-control measures. Workers, in turn, are more likely to be upset about employer efforts at health care cost control (such as lower negotiated provider and drug prices) because they are not aware that the lack of cost control leads directly to higher premiums and lower wages.
- Disincentives for insurers to control costs. Insurers’ operating margins are relatively constant over time, and regulated at the federal and state levels. If an insurer is effectively required to keep its operating margin at 10 percent, for example, the best way for the insurer to grow its operating income over time is to collect higher premiums over time. In other words, insurers in the employer market are incentivized to encourage health care inflation, because 10 percent of a bigger number is more income for them. This incentive is weaker in the non-group (i.e., non-employer) market for health insurance, because workers’ price sensitivity rewards lower-cost insurance.
- Health insurance mission creep. To use an analogy, we do not use auto insurance to pay for routine items like gasoline or oil changes. But because the tax code heavily rewards spending on health insurance over other forms of personal spending, we now think of health insurance as a vehicle for any and all kinds of health care products and services, even if those services or products do not comprise what we normally think of as insurable events. As more and more products and services are covered by health insurance, those additional items also participate in rapid health care inflation.
It has become common for health care commentators to talk about “eliminating the middlemen” from health care. There is no costlier middleman than employers.
The high cost of U.S. health care also worsens American health outcomes. There is considerable literature indicating that the high cost of health care leads patients to avoid routine care and to use prescription drugs less frequently than medically recommended. Also, rising health care costs for employers lead to lower rates of employment, increasing deaths of despair from suicides and overdoses.
The Swiss model: Universal, individually purchased insurance
As noted above, there are numerous alternatives to single-payer health care for achieving lower costs and better outcomes. The FREOPP World Index of Healthcare Innovation ranks 32 high-income countries along dozens of measures of quality, choice, science & technology, and fiscal sustainability.
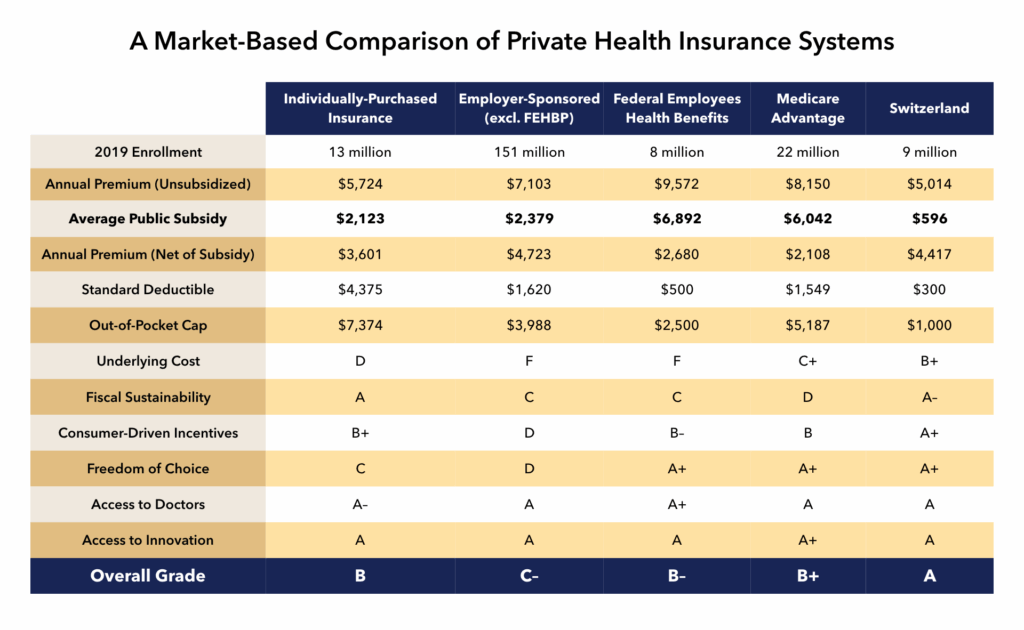
In each year of the survey, Switzerland has ranked first overall. In 2024, Switzerland ranked 2nd in Quality, 2nd in Choice, 2nd in Science & Technology, and 3rd in Fiscal Sustainability. Notably, Switzerland does not have single-payer health care, but rather a system of universal, individually-purchased health insurance, similar in important ways to Medicare Advantage (the market for private insurers who deliver the Medicare benefit to seniors) and the Affordable Care Act’s (Obamacare’s) insurance marketplaces . As befitting a nation famous for precision engineering, Switzerland’s individual insurance marketplace produces results that are superior to the Affordable Care Act’s.
The median monthly premium for a benchmark ACA Silver plan in 2026 is $625, compared to $586 (CHF 465.30) in Switzerland. The median deductible for an ACA Silver plan in 2026 is $5,300, compared to around $375 (CHF 300). Compared to single-payer systems, Swiss consumers enjoy broad freedom of choice in both insurers and doctors, and access to the latest medical technologies, many of which originate from Swiss-based companies.
Why are Swiss plans more affordable, with better outcomes, than ACA plans? The biggest reason is that 80 years of U.S. health care inflation driven by the ESI exclusion have led to significantly higher unit prices in the U.S. relative to Switzerland. Since we cannot rewind history, it is not so easy to simply wipe out the longstanding policy impact of the ESI exclusion.
But it is never too late to start a voluntary, gradual migration away from employer-sponsored insurance and into individually purchased coverage. In order to do so, we must repair the ACA’s biggest design flaws, so that individually purchased coverage can become a superior option to employer-based coverage. In addition, we can learn from the Swiss health care system to lower costs and improve outcomes for all Americans.
Repairing the ACA’s biggest flaws
While ACA insurance premiums are lower than those for employer-sponsored insurance, their prices are rapidly rising, due to a structure of regulations and subsidies that discourage younger and healthier individuals from enrolling.
- Overcharging the young. The ACA made health insurance less affordable for Americans in their 30s and late 20s by preventing insurers from charging young people a lower premium. Specifically, the ACA forbids insurers from giving young people more than a 67 percent discount relative to what insurers charge their oldest customers. As a result, young people drop out of the market, making health insurance costlier for everyone, including those in their 60s. A simple measure increasing the allowable discount to 80 percent — a 5-to-1 “age band” — could largely fix this problem. More young people would enroll, improving the quality of the risk pool and thereby reducing premiums for the young and old alike. Congress could also age-adjust the ACA subsidy formula to make absolutely sure that premiums for older enrollees stayed the same.
- Overcharging the healthy. A related flaw in the ACA is that it requires insurers to overcharge healthy people in order to (theoretically) undercharge those with preexisting conditions. Again, this encourages healthy people to drop out of the market, raising premiums for everyone who remains. A bipartisan reform package could fix this by creating a $10 billion-per-year reinsurance fund that would directly subsidize premiums for the sick and the chronically ill, while leaving protections for those with preexisting conditions unchanged. The reinsurance program could deploy innovative value-based strategies to address chronic metabolic and cardiovascular diseases like diabetes and coronary artery disease.
- Lack of appropriations for cost-sharing reduction subsidies. A drafting error in the ACA has resulted in increased Silver premiums—commonly called Silver loading—because insurers are required to offer low-deductible plans to low-income enrollees, but are not currently compensated by the federal government for the extra cost for doing so. A Congressional appropriation for these cost-sharing reduction subsidies would enable insurers to reduce premiums for Silver plans. In 2018, the Congressional Budget Office estimated that appropriating CSRs would reduce the deficit by $29 billion over ten years, because reducing ACA premiums would also reduce the cost of subsidizing ACA premiums.
- Facilitate employer funding of individually purchased insurance. The ACA requires employers with more than 50 full-time workers to sponsor traditional employer coverage. But workers would benefit from a repeal of this mandate, and a codification of rules enabling employers to fund Individual Coverage Health Reimbursement Arrangements, or ICHRAs.
- Arbitrary churn between Medicaid and individual coverage. The authors of the ACA believed that Medicaid-based coverage would be a less costly way for low-income able-bodied uninsured adults to gain health insurance. But in fact, ACA-based coverage is now less costly than the Medicaid expansion. In addition, under the ACA, low-income adults with volatile incomes end up churning between Medicaid-based coverage and ACA marketplace-based coverage, with different premiums and provider networks. We estimate that migrating able-bodied adults on the ACA Medicaid expansion into the exchanges would save $159 billion over a decade.
- Program integrity issues. A recent investigation by the U.S. Government Accountability Office found that “the federal Marketplace approved coverage for nearly all of GAO’s fictitious applicants in plan years 2024 and 2025, generally consistent with similar GAO testing in plan years 2014 through 2016.” Better verification technology can help, as can reforms that benchmark ACA subsidies to prior-year tax returns, as opposed to estimated future income.
Learning from the Swiss model
There are several additional reforms Congress could enact in order to lower costs and improve health outcomes.
- Longer health insurance contracts. Switzerland gives consumers the option of supplemental insurance contracts that last up to five years. The problem with standard one-year enrollment periods is that insurers lack the incentive to invest in long-term prevention, because they are unlikely to reap the rewards of those investments if patients switch insurers later on. Swiss insurers, by contrast, can benefit economically from prevention. Some offer 50 percent refunds if enrollees meet certain targets for common laboratory measures like blood pressure or hemoglobin A1c.
- Trade association-based price negotiation. Switzerland has developed sophisticated mechanisms for combating the pricing power of health care monopolies, such as regional hospital systems and branded pharmaceuticals. Within a given canton (the Swiss equivalent of a U.S. state), insurers are able to jointly negotiate reimbursement rates, alongside the trade associations for hospitals, physicians, pharmaceutical companies, and the like.
- Migrating FEHB participants into the individual market. Congress could strengthen the individual market for health insurance by migrating enrollees in the Federal Employee Health Benefits Program into the ACA marketplaces. In 2025, the average monthly premium for an FEHB plan was $897 for self-only coverage, compared to $497 for the median ACA Silver plan. We estimate that a full transition could reduce the deficit by over $10 billion per year in reduced subsidies and regained tax revenue. Doing so would also double the size of the individual market, creating economies of scale whereby more insurers would participate and compete with each other, lowering premiums and increasing quality.
Strengthening health outcomes through payment innovation
The way we pay for health care profoundly retards our ability to develop innovative approaches to health care delivery. Opening health care to novel approaches require us to liberalize the way we pay for health care, such as by enabling longer-term insurance contracts. Direct primary care has proven to be a successful model for reducing adverse clinical events for the elderly and near-elderly.
In particular, the Medicare and Medicaid programs are in many ways ossified by their 1965 design. One way to substantially open up innovation in health delivery would be to exempt from Medicare the wealthiest 5 to 10 percent of future seniors born after 1970, in terms of lifetime earnings. (The Social Security Administration already calculates lifetime earnings, making this an easily administrable test that is difficult to game.) As a matter of fairness, low- and middle-income Americans should not be paying taxes to fund Medicare for the wealthiest. And requiring the wealthiest seniors to obtain coverage and care on their own would open up a market of 6 million seniors to innovators and entrepreneurs who could reimagine the delivery of health care to this population using 21st-century tools.
Too often, the U.S. health care debate centers around spending more money or less money but not reforming the underlying system. The good news is that with well-designed reforms, it is possible to lower costs, improve coverage, and increase health care outcomes at the same time.
(Note: This paper is adapted from testimony Avik Roy delivered to the U.S. Congress Joint Economic Committee on December 17, 2025.)
